

Psoriatic Arthritis
Psoriatic arthritis affects both men and women equally and usually develops between the ages of 20 – 50. There are over 1 million people in the United
States that have psoriatic arthritis. There are many different sub-types of psoriatic arthritis, so it is important to see your rheumatologist for the correct
diagnosis. The joint pains caused by psoriatic arthritis commonly affect the fingers, wrists, toes, ankles, knee and low back. The low back “pain” associated
with psoriatic arthritis may be described as back stiffness, which is worse in the morning or after periods of inactivity and improves with stretching exercises.
Most adults with degenerative disc disease, a very common form of arthritis, are “ok” in the morning or after periods of inactivity, but have more back pain with
activity. Psoriasis may also cause “fungus like” changes of your finger and toenails.
In up to 25% of the cases of psoriatic arthritis, the patient develops the arthritis first, BEFORE developing the skin rash (psoriasis) and this may make the
proper diagnosis more difficult. If you have a first degree relative (mother, father, brother or sister) with psoriasis or psoriatic arthritis, you are at increased
risk of developing similar medical problems.
What causes psoriatic arthritis?
The cause of psoriatic arthritis is not known. As with all autoimmune problems, it is believed that a trigger (stress, infection) in a person with a genetic
predisposition, leads to an abnormal, overactive immune response, which then causes psoriatic arthritis. Your immune system is made up of blood cells
that usually protect you from infections and pre-cancerous cells. When the body’s immune system starts to attack the body itself, it is called an autoimmune
disease. Psoriatic arthritis is one of many autoimmune diseases that rheumatologist are specially trained to diagnose and treat. Other forms of
autoimmune diseases include rheumatoid arthritis and lupus.
What are the symptoms of psoriasis and psoriatic arthritis?
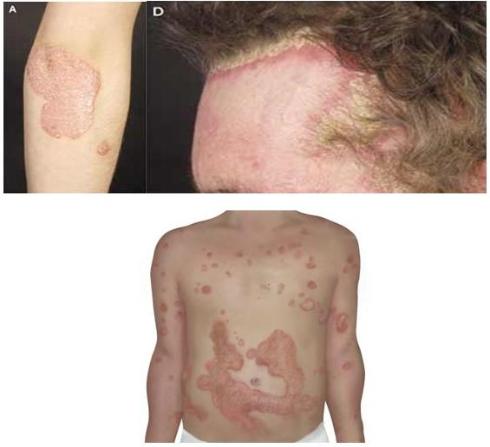
1) Silver or grey, scaly spots on the scalp, elbows, knees and or low back area.
2) Pitting (small depressions) or thickening of the finer and or toenails. Your nails may look like they are pulling away from the fingers.
3) Swelling & pain in one or more joints in the fingers, wrists, toes, ankles or knees. Heel pain, plantar fasciitis and recurrent trigger fingers.
4) Swelling of the fingers and or toes that give them a “sausage-like” appearance.
5) Low back (or buttock) pain and or stiffness which worsens after periods of inactivity and improves with stretching.
6) Extra-Articular Manifestations: Psoriatic Arthritis is associated with inflammation of other organs besides the joints like:
a. Red, itchy, light sensitive eyes (Iritis, Uveitis)
b. Blood in your stools (Inflammatory bowel disease: Crohn’s disease or Ulcerative Colitis)
The course of psoriatic arthritis varies; patients have good and bad days. The extent of the psoriasis does NOT correlate with the extent and or damage of
the arthritis. Said anther way, you do NOT need to have BAD psoriasis to have psoriatic arthritis and similarly, people with BAD psoriatic arthritis do NOT
always have BAD skin disease.
What are the patterns of joint involvement?
When psoriatic arthritis begins, it may only involve one or two joints on different sides of the body (asymmetric). As psoriatic arthritis progresses, more and
more joints may become involved and affect both sides of the body (symmetric), which is typically how rheumatoid arthritis presents. Five to 10% of patients
with psoriatic arthritis can have a low positive RF blood test, confusing the diagnosis. Some of the unique features of psoriatic arthritis that distinguishes it
from RA, include the development of swollen fingers and or toes (sausage digits) and spondylitis (inflammatory low back arthritis).
Fortunately, the most debilitating form of psoriatic arthritis is also the least common form, called arthritis mutilans, which occurs in less than 5% of psoriatic
arthritis patients. In arthritis mutilans, the joints of the hands are completely destroyed, which causes the patient to be very disabled. One of the most
important goals in the early diagnosis and treatment of psoriatic arthritis, is to prevent bone damage because once established, the joint damage cannot be
reversed with medications.
How is psoriatic arthritis diagnosed?
The diagnosis of psoriatic arthritis requires a full history, physical examination in addition to blood work and x-rays. Your rheumatologist will examine your
skin for psoriasis on your skin or psoriasis nail changes in addition to looking for swelling, tenderness and limitation of motion of your joints. Blood tests
are needed to rule out other kinds of arthritis, like rheumatoid arthritis and lupus, and to establish your baseline blood count, liver and kidney function along
with blood markers of inflammation. X-rays are used to assess joint damage as seen below.
How is psoriatic arthritis treated?
The goal of treatment of psoriatic arthritis is to control the skin rash, control the joint pain and swelling and to prevent joint damage and physical disability.
You may have a dermatologist (skin specialist) and a rheumatologist working together to optimize your treatment goals. No single treatment works for
everyone.
To treat your skin disease (psoriasis), your dermatologist may recommend several treatment options including: 1) keeping your skin from becoming dry, 2)
topical steroid creams and 3) light box treatments. Unfortunately, these treatment options for your skin do not help treat or prevent joint damage.
To treat your psoriatic arthritis, your rheumatologist may recommend several treatment options including: 1) NSAIDS, 2) methotrexate or 3) the anti-TNF
agents. NSAIDS are the Non Steroidal Anti-Inflammatory DrugS like aspirin, ibuprofen and naproxen, which can help reduce joint pains and swelling. Low
doses of these types of medication are available over the counter while higher doses are available only by prescription. Although these medications are
helpful in reducing the pain and swelling of psoriatic arthritis, they do NOT prevent structural bone damage and disability that occur over many years of active
psoriatic arthritis.
Methotrexate is a DMARD (Disease Modifying Anti-Rheumatic Drug) medication used in the treatment of both psoriasis and psoriatic arthritis. In addition to
reducing the pain, swelling and stiffness of psoriatic arthritis, methotrexate can also improve the psoriatic skin lesions and prevent structural bone damage
and its associated physical disability. While on methotrexate, you must not drink alcohol and if you are of child bearing age, you must use at least two forms
of birth control. Methotrexate and alcohol can both irritate the liver and methotrexate is a teratogen (drug that causes birth defects). For more information on
methotrexate, please see our drug webpage.
The Tumor Necrosis Factor (TNF) inhibitors, etanercept (Enbrel), infliximab (Remicade) and adalimumab (Humira), are all FDA approved for the treatment of
psoriasis and psoriatic arthritis. Enbrel and Humira are self administered injections and Remicade is an IV infusion. In addition to clearing up the
psoriasis, these agents also decrease the pain, swelling and prevent bone damage associated with psoriatic arthritis.
The most common side effects are a local injection site rash, which is usually mild and temporary, or slight light headedness with the IV infusion if given too
quickly. To prevent any side effects with the Remicade IV infusion, it is given slowly over two hours under the supervision of a nurse. Before starting any anti-
TNF agent, you will need to have a PPD skin test to check to see if you have been exposed to tuberculosis (TB) in the past. If you have been exposed to TB in
the past, you will need to take a medication prior to beginning any anti-TNF agent to prevent the TB from becoming active while on treatment. Please talk to
your rheumatologist regarding other precautions in the use of the anti-TNF agents.
Exercise & Rest
Exercise is an important part of your treatment plan. It can limit the pain, swelling and limitation of motion of your affected joints and can also improve your
muscle strength, improve your sleep and your overall sense of well being. If your arthritis is flaring, simple range-of-motion exercises without weights are
good to do to maintain a normal range of motion of the joints. When your arthritis is under better control, you can slowly increase the intensity and duration.
Work with your rheumatologist and physical therapist to develop an exercise program that is right for you.
Generally, normal amounts of rest and sleep are sufficient to decrease your fatigue and reduce your joint inflammation.
References:
www.arthritis.org
www.psoriasis.org
Psoriatic arthritis affects both men and women equally and usually develops between the ages of 20 – 50. There are over 1 million people in the United
States that have psoriatic arthritis. There are many different sub-types of psoriatic arthritis, so it is important to see your rheumatologist for the correct
diagnosis. The joint pains caused by psoriatic arthritis commonly affect the fingers, wrists, toes, ankles, knee and low back. The low back “pain” associated
with psoriatic arthritis may be described as back stiffness, which is worse in the morning or after periods of inactivity and improves with stretching exercises.
Most adults with degenerative disc disease, a very common form of arthritis, are “ok” in the morning or after periods of inactivity, but have more back pain with
activity. Psoriasis may also cause “fungus like” changes of your finger and toenails.
In up to 25% of the cases of psoriatic arthritis, the patient develops the arthritis first, BEFORE developing the skin rash (psoriasis) and this may make the
proper diagnosis more difficult. If you have a first degree relative (mother, father, brother or sister) with psoriasis or psoriatic arthritis, you are at increased
risk of developing similar medical problems.
What causes psoriatic arthritis?
The cause of psoriatic arthritis is not known. As with all autoimmune problems, it is believed that a trigger (stress, infection) in a person with a genetic
predisposition, leads to an abnormal, overactive immune response, which then causes psoriatic arthritis. Your immune system is made up of blood cells
that usually protect you from infections and pre-cancerous cells. When the body’s immune system starts to attack the body itself, it is called an autoimmune
disease. Psoriatic arthritis is one of many autoimmune diseases that rheumatologist are specially trained to diagnose and treat. Other forms of
autoimmune diseases include rheumatoid arthritis and lupus.
What are the symptoms of psoriasis and psoriatic arthritis?
1) Silver or grey, scaly spots on the scalp, elbows, knees and or low back area.
2) Pitting (small depressions) or thickening of the finer and or toenails. Your nails may look like they are pulling away from the fingers.
3) Swelling & pain in one or more joints in the fingers, wrists, toes, ankles or knees. Heel pain, plantar fasciitis and recurrent trigger fingers.
4) Swelling of the fingers and or toes that give them a “sausage-like” appearance.
5) Low back (or buttock) pain and or stiffness which worsens after periods of inactivity and improves with stretching.
6) Extra-Articular Manifestations: Psoriatic Arthritis is associated with inflammation of other organs besides the joints like:
a. Red, itchy, light sensitive eyes (Iritis, Uveitis)
b. Blood in your stools (Inflammatory bowel disease: Crohn’s disease or Ulcerative Colitis)
The course of psoriatic arthritis varies; patients have good and bad days. The extent of the psoriasis does NOT correlate with the extent and or damage of
the arthritis. Said anther way, you do NOT need to have BAD psoriasis to have psoriatic arthritis and similarly, people with BAD psoriatic arthritis do NOT
always have BAD skin disease.
What are the patterns of joint involvement?
When psoriatic arthritis begins, it may only involve one or two joints on different sides of the body (asymmetric). As psoriatic arthritis progresses, more and
more joints may become involved and affect both sides of the body (symmetric), which is typically how rheumatoid arthritis presents. Five to 10% of patients
with psoriatic arthritis can have a low positive RF blood test, confusing the diagnosis. Some of the unique features of psoriatic arthritis that distinguishes it
from RA, include the development of swollen fingers and or toes (sausage digits) and spondylitis (inflammatory low back arthritis).
Fortunately, the most debilitating form of psoriatic arthritis is also the least common form, called arthritis mutilans, which occurs in less than 5% of psoriatic
arthritis patients. In arthritis mutilans, the joints of the hands are completely destroyed, which causes the patient to be very disabled. One of the most
important goals in the early diagnosis and treatment of psoriatic arthritis, is to prevent bone damage because once established, the joint damage cannot be
reversed with medications.
How is psoriatic arthritis diagnosed?
The diagnosis of psoriatic arthritis requires a full history, physical examination in addition to blood work and x-rays. Your rheumatologist will examine your
skin for psoriasis on your skin or psoriasis nail changes in addition to looking for swelling, tenderness and limitation of motion of your joints. Blood tests
are needed to rule out other kinds of arthritis, like rheumatoid arthritis and lupus, and to establish your baseline blood count, liver and kidney function along
with blood markers of inflammation. X-rays are used to assess joint damage as seen below.
How is psoriatic arthritis treated?
The goal of treatment of psoriatic arthritis is to control the skin rash, control the joint pain and swelling and to prevent joint damage and physical disability.
You may have a dermatologist (skin specialist) and a rheumatologist working together to optimize your treatment goals. No single treatment works for
everyone.
To treat your skin disease (psoriasis), your dermatologist may recommend several treatment options including: 1) keeping your skin from becoming dry, 2)
topical steroid creams and 3) light box treatments. Unfortunately, these treatment options for your skin do not help treat or prevent joint damage.
To treat your psoriatic arthritis, your rheumatologist may recommend several treatment options including: 1) NSAIDS, 2) methotrexate or 3) the anti-TNF
agents. NSAIDS are the Non Steroidal Anti-Inflammatory DrugS like aspirin, ibuprofen and naproxen, which can help reduce joint pains and swelling. Low
doses of these types of medication are available over the counter while higher doses are available only by prescription. Although these medications are
helpful in reducing the pain and swelling of psoriatic arthritis, they do NOT prevent structural bone damage and disability that occur over many years of active
psoriatic arthritis.
Methotrexate is a DMARD (Disease Modifying Anti-Rheumatic Drug) medication used in the treatment of both psoriasis and psoriatic arthritis. In addition to
reducing the pain, swelling and stiffness of psoriatic arthritis, methotrexate can also improve the psoriatic skin lesions and prevent structural bone damage
and its associated physical disability. While on methotrexate, you must not drink alcohol and if you are of child bearing age, you must use at least two forms
of birth control. Methotrexate and alcohol can both irritate the liver and methotrexate is a teratogen (drug that causes birth defects). For more information on
methotrexate, please see our drug webpage.
The Tumor Necrosis Factor (TNF) inhibitors, etanercept (Enbrel), infliximab (Remicade) and adalimumab (Humira), are all FDA approved for the treatment of
psoriasis and psoriatic arthritis. Enbrel and Humira are self administered injections and Remicade is an IV infusion. In addition to clearing up the
psoriasis, these agents also decrease the pain, swelling and prevent bone damage associated with psoriatic arthritis.
The most common side effects are a local injection site rash, which is usually mild and temporary, or slight light headedness with the IV infusion if given too
quickly. To prevent any side effects with the Remicade IV infusion, it is given slowly over two hours under the supervision of a nurse. Before starting any anti-
TNF agent, you will need to have a PPD skin test to check to see if you have been exposed to tuberculosis (TB) in the past. If you have been exposed to TB in
the past, you will need to take a medication prior to beginning any anti-TNF agent to prevent the TB from becoming active while on treatment. Please talk to
your rheumatologist regarding other precautions in the use of the anti-TNF agents.
Exercise & Rest
Exercise is an important part of your treatment plan. It can limit the pain, swelling and limitation of motion of your affected joints and can also improve your
muscle strength, improve your sleep and your overall sense of well being. If your arthritis is flaring, simple range-of-motion exercises without weights are
good to do to maintain a normal range of motion of the joints. When your arthritis is under better control, you can slowly increase the intensity and duration.
Work with your rheumatologist and physical therapist to develop an exercise program that is right for you.
Generally, normal amounts of rest and sleep are sufficient to decrease your fatigue and reduce your joint inflammation.
References:
www.arthritis.org
www.psoriasis.org
Disease Information

Psoriasis Finger Nail
Pitting
Pitting



Psoriatic Arthritis of the Hands
with Thickening of the
Fingernails due to Psoriasis.
“sausages” with thickening of
the toe nails.the toe nails.

Same patient AFTER two
months of anti-TNF
treatment.
